Access Menu
What is peripheral vascular disease?
 Peripheral vascular disease, or PVD, is a condition in which the arteries that carry blood to the arms or legs become narrowed or clogged, interfering with the normal flow of blood. The most common cause of PVD is atherosclerosis (often called hardening of the arteries). Atherosclerosis is a gradual process in which cholesterol and scar tissue build up, forming a substance called “plaque” that clogs the blood vessels. PVD may also be caused by blood clots.
Peripheral vascular disease, or PVD, is a condition in which the arteries that carry blood to the arms or legs become narrowed or clogged, interfering with the normal flow of blood. The most common cause of PVD is atherosclerosis (often called hardening of the arteries). Atherosclerosis is a gradual process in which cholesterol and scar tissue build up, forming a substance called “plaque” that clogs the blood vessels. PVD may also be caused by blood clots.
What are the symptoms of PVD?
PVD Symptoms
- Leg or hip pain during walking
- The pain stops when you rest
- Numbness
- Tingling
- Weakness in the legs
- Burning or aching pain in feet or toes when resting
- Sore on leg or foot that won’t heal
- Cold legs or feet
- Color change in skin of legs or feet
- Loss of hair on legs
The disease, which affects both men and women, often goes undiagnosed and many people mistakenly think the symptoms are a normal part of aging.
The most common symptom of PVD is called intermittent claudication, a painful cramping in the leg or hip, particularly when walking. Intermittent claudication occurs when there is not enough blood flowing to the leg muscles during exercise. The pain typically goes away when the muscles are given a rest.
Other symptoms may include numbness, tingling or weakness in the leg. In severe cases, you may experience a burning or aching pain in the feet or toes while resting, or develop a sore on the leg or foot that does not heal. People with PVD may also experience a cooling or color change in the skin of the legs or feet, or loss of hair on the legs. In extreme cases, untreated PVD can lead to gangrene, a serious condition that may require amputation of a leg or a foot.
If you have PVD, you are also at higher risk for heart disease and stroke.
Who is at risk for PVD and intermittent claudication?
As many as 10 million people in the U.S. may have PVD. It is estimated that 4 million of those suffer leg pain symptoms. Those who are at highest risk are:
- over the age of 50,
- smokers,
- diabetic,
- overweight,
- people who do not exercise, or
- people with high blood pressure or high cholesterol.

A family history of heart or vascular disease may also put you at higher risk for PVD.
How is PVD diagnosed?
The most common test for PVD is the ankle-brachial index (ABI), a painless exam in which ultrasound is used to measure the ratio of blood pressure in the feet and arms. Based on the results of your ABI, as well as your symptoms and risk factors
for PVD, the physician can decide if further tests are needed. PVD also can be diagnosed noninvasively with an imaging technique called magnetic resonance angiography (MRA), or with computed tomography (CT) angiography.
How can PVD be treated?
The best treatment for PVD depends on a number of factors, including your overall health and the severity of the disease. In some cases, lifestyle changes are enough to halt the progression of PVDand manage the disease. Your physician may prescribe drugs when lifestyle changes are not enough. Procedures that open clogged blood vessels also are used to treat PVD.
Lifestyle changes. Most treatment plans will include a low fat diet and a program of regular exercise. If you are a smoker, it is absolutely essential that you stop the use of all types of tobacco. If decreased blood flow to the legs is causing injury to the feet and toes, a foot care program to prevent sores or infection may be prescribed. This may include referral to a podiatrist.
Medication. Medications that lower cholesterol or control high blood pressure may be prescribed. Medication also is available that has been shown to significantly increase pain-free walking distance and total walking distance in people with intermittent claudication. Other medications that help prevent blood clots or the build-up of plaque in the arteries are available, as well.
What can be done to treat PVD when lifestyle changes and medications are not enough?
 There are a number of ways that physicians can open blood vessels at the site of blockages and restore normal blood flow. In many cases, these procedures can be performed without surgery using modern, interventional radiology techniques. Interventional radiologists are physicians who use tiny tubes called catheters and other miniaturized tools, and X-rays to do these procedures.
There are a number of ways that physicians can open blood vessels at the site of blockages and restore normal blood flow. In many cases, these procedures can be performed without surgery using modern, interventional radiology techniques. Interventional radiologists are physicians who use tiny tubes called catheters and other miniaturized tools, and X-rays to do these procedures.Procedures performed by interventional radiologists include:
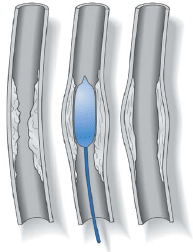
- angioplasty – a balloon is inflated to open the blood vessel.
- thrombolytic therapy – clot-busting drugs are delivered to the site of blockages caused by blood clots.
- stents – a tiny metal cylinder, or stent, is inserted in the clogged vessel to act like a scaffolding and hold it open.
- stent-grafts – a stent covered with synthetic fabric is inserted into the blood vessels to bypass diseased arteries.
Sometimes, open surgery is required to remove blockages from arteries or to bypass the clogged area. These procedures are performed by vascular surgeons.
How can I find out if I have PVD?
If you suspect that you may have PVD, it is important that you see your personal physician for an evaluation.